Vein Clinic Minneapolis
Live An Active Life With Healthy, Pain Free Legs.
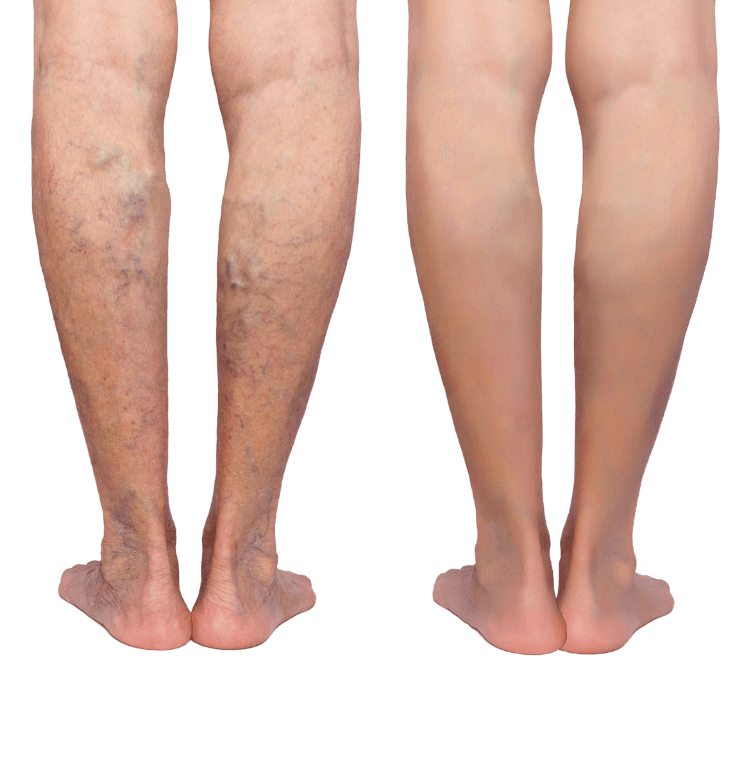
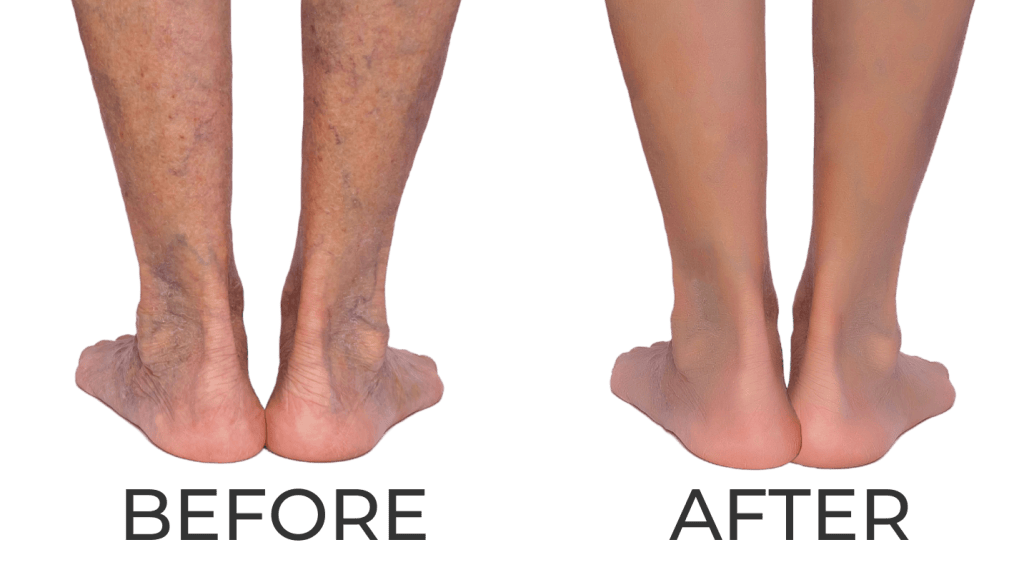
Do You Experience…
- Skin Changes / Discoloration
- Leg Pain / Aching / Cramping
- Leg Heaviness and Fatigue
- Restless Legs
- Leg Itching / Burning / Numbness
- Skin Changes or Rashes
- Ulcers / Open Wounds / Sores
- Varicose Veins
If so, you may be eligible for non-invasive varicose vein treatment.
What is Vein Disease? Why do I have it?
Dr. Kalsi shares the top three reason why you may get vein disease. Watch the video to learn more!
What is Vein Disease? Why do I have it?
Dr. Kalsi shares the top three reason why you may get vein disease. Watch the video to learn more!
Trusted by Patients Across Minnesota
Insurance
Virtually Painfree
We’re equipped with the latest cutting-edge, minimally invasive, and virtually pain-free vein treatments!
Quick Recovery
You’ll be surprised how most of our patients return to their normal day-to-day activities the very same day!
15-45 Minutes
Why Minnesota Vein Clinic?
Why You Shouldn't Leave Your Varicose Veins Untreated
- Persistent Pain: Varicose veins contribute to venous reflux, disrupting proper blood circulation and leading to diminished oxygen delivery, resulting in muscle cramps and localized pain.
- Risk of Infection: Venous conditions may lead to the development of leg ulcers, increasing susceptibility to skin lesions and potential complications due to exposure to bacteria.
- Bleeding: Varicose veins, located closer to the skin’s surface and prone to inflammation, are more susceptible to injury and subsequent bleeding incidents.
- Swelling: Hindered blood flow within the legs can cause reflux, resulting in swelling and discomfort due to inefficient circulation.
- Blood Clots: Blood pooling in the legs heightens the risk of clot formation, which could dislodge and travel through the bloodstream, potentially triggering serious conditions such as deep vein thrombosis and pulmonary embolism (PE).
About Minnesota Vein Center

Identify, Treat, and Eliminate
Minnesota Vein Center is a highly specialized medical practice dedicated to providing the most advanced chronic venous insufficiency, varicose vein, and spider vein treatment in Minnesota. Our vein clinic has three convenient locations near Minneapolis. We provide comprehensive vein care in a comfortable clinic environment, including expert consultation with vein specialists and state-of-the-art, minimally invasive treatments.
Visit One of Our Minnesota Vein Center Locations!
FAQs
Most Frequent Questions and Answers
What are Varicose Veins? What are Spider Veins?
In your leg, you have two sets of veins. They are called deep veins and superficial veins.
Deep veins are in the deeper part of the leg where the muscles are, and superficial veins are right under the skin.
In a normal person, the blood circulates from the feet toward the heart in both veins.
When someone has venous insufficiency, the blood will go up the deep veins and back into the superficial vein.
The blood will start pooling in the superficial veins.
Since the superficial veins are closest to the skin, they will bulge and create varicose veins. Varicose veins are abnormally enlarged veins in the legs that are sometimes ropy and twisted in appearance.
Spider veins are groups of red or blue veins, close to the surface of the skin, that resemble the delicate strands of spider webs. Spider Veins are essentially a smaller version of varicose veins. They are most often seen on the legs, chest, or face.. It is common to find spider veins and varicose veins together.
Do Varicose Veins ALWAYS Show Physical Symptoms?
No. Varicose veins can occur deeper in the leg, where one can’t see them. Varicose veins are classified under the spectrum of venous insufficiency.
Venous insufficiency causes leg discomfort, swelling of the ankles and leg, itching, and fatigue. Other signs and symptoms may be prickling, cramping, aching, and heaviness of the lower limbs after prolonged standing.
Keep an eye out for these symptoms besides simply visible veins.
Can I Get Rid of Varicose Veins Naturally?
What Happens If I Don’t Treat Varicose Veins?
Progression of varicose veins can be dangerous as they may later become venous ulcerations. When left without treatment, complications may include rashes, infections, bleeding, sores, and blood clots.
In rare cases, varicose veins can cause deep vein thrombosis (DVT) and pulmonary embolism, which is life-threatening.
What is Your Process? How are Varicose Veins Diagnosed?
1) Consult – We start you with a consultation where you will be listened to and encounter a friendly staff that will ensure you get the best care. On the first visit, that care will come from our expertly trained team, including Dr. Kalsi and an ultrasonographer.
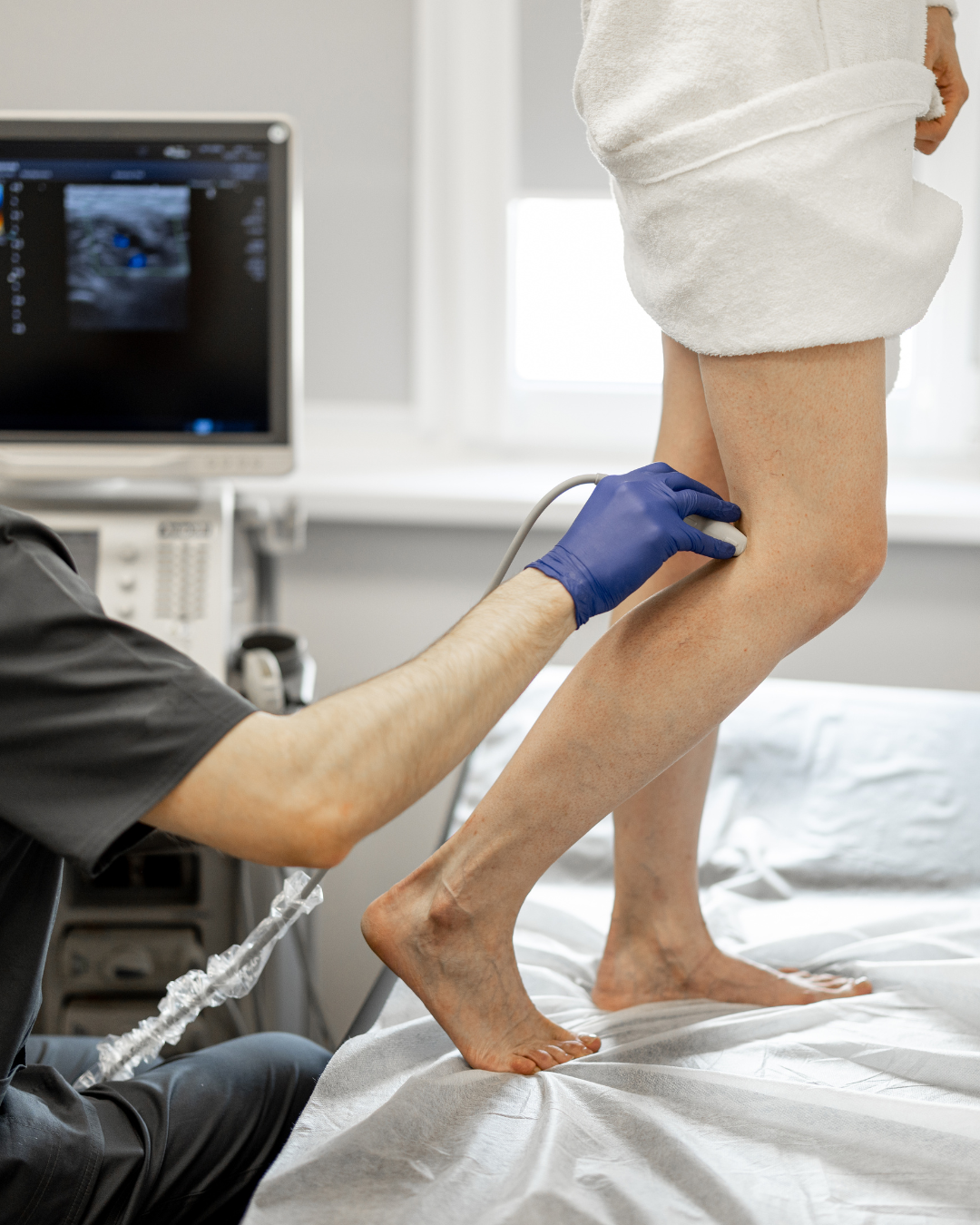
2) Ultrasound – After the consult, we move on to the assessment, providing you with an accurate diagnosis. You will get the same-day ultrasound and results on-site while you see the provider. This will get you back to life as swiftly as possible.
3) Treatment Plan – After we conclude our assessment, we will provide you with a treatment plan.
There are many different options, such as Radiofrequency Ablation (RFA), sclerotherapy, pneumatic compression, and more. We will ensure you get the perfect customized treatment based on your needs and outcome goals.
Does the Treatment Hurt?
How Long Does it Take to Recover From Varicose Vein Treatment?
Patients usually return to work and activities on the very same day. Very little downtime is needed for our treatments.
Payment Policies

